Does a Normal Blood Test Really Mean You're Fine? Here's the Truth
- Dr Hassan Paraiso
- Mar 19
- 6 min read
You've been feeling exhausted for months. Perhaps you're short of breath climbing the stairs, or you've noticed your hair thinning, or you simply don't feel like yourself. So you see your GP, they run a battery of blood tests, and a week later the results come back: "Everything's normal."
But here's the thing, you still feel dreadful.
If this sounds familiar, you're not alone. It's one of the most common frustrations I hear in my practice: patients who know something is wrong but are told their tests are fine. The truth is, a "normal" blood test doesn't always mean you're healthy, and understanding why can be the first step toward getting proper answers.
What does "normal" actually mean?
When your doctor says your blood test is normal, what they really mean is that your results fall within a statistical range called a "reference range". This range is calculated by testing large numbers of people and defining normal as the middle 95% of results, in other words, where most people sit.
The crucial word here is "most". A normal result tells you that your levels are similar to the general population. It doesn't tell you whether those levels are optimal for you, whether you're at the high or low end of that range, or whether your symptoms might be explained by something the test didn't measure.
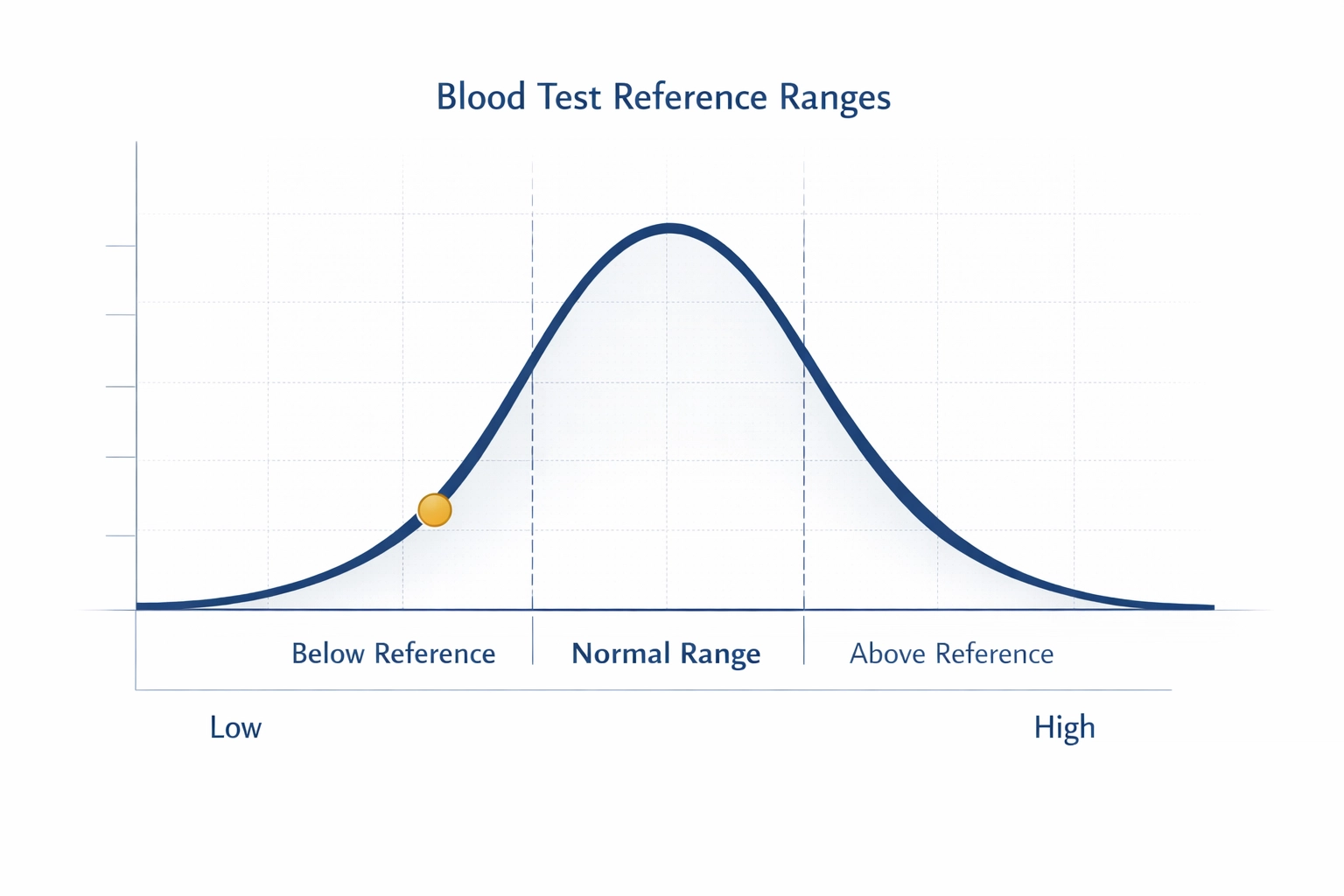
Think of it this way: if you're usually a marathon runner but you're now struggling to jog around the block, telling you that your heart rate is "normal compared to the average person" misses the point entirely. Context matters.
The problem with reference ranges
Reference ranges have several significant limitations that most patients aren't aware of.
They reflect the population tested, not optimal health
The original blood samples used to create reference ranges often came from whoever happened to be having blood tests at the time, not necessarily a group of optimally healthy people. If the population being tested includes many people with subclinical deficiencies or early disease, the "normal" range shifts to reflect that less-than-ideal baseline.
Take vitamin D as an example. Studies show that 42% of adults in the UK have insufficient or deficient levels. When that many people are low, the reference range starts to reflect widespread deficiency rather than what's genuinely healthy. You could have vitamin D levels that are "normal" but still far below what your body needs to function at its best.
Ranges change over time, and not always for good reasons
Men's testosterone levels have been steadily declining for decades across Western populations. As average levels drop, reference ranges are adjusted downward to match. A level that would have been flagged as low 30 years ago might now be considered normal, not because we understand testosterone better, but simply because more men now have lower levels.
They don't account for individual variation
Some people naturally run at the high end of normal for certain markers; others run low. If your thyroid function has always been at the top of the range and it drops to the bottom, but still technically normal, you might feel significantly different, even though the numbers look fine on paper.
Different labs, different results
Here's something that surprises many patients: the same blood sample can produce different results depending on which laboratory analyses it.
Laboratories use different equipment, different methodologies, and calculate their own reference ranges based on their local populations. This means you could test as "normal" at one lab and "abnormal" at another, even though nothing about your health has changed.
This variation isn't necessarily a sign of poor quality, it's simply a reflection of how these tests work. But it does mean that fixating on whether a number is just inside or just outside the reference range can be misleading. What matters more is the trend over time and how the results fit with your symptoms.

Test accuracy matters
Even when performed correctly, no blood test is 100% accurate at detecting disease.
Every test has two important measures:
Sensitivity: how good it is at correctly identifying disease when it's present. A test with 70% sensitivity will miss 30% of people who actually have the condition (false negatives).
Specificity: how good it is at correctly confirming absence of disease. Poor specificity leads to false positives, being told you have a problem when you don't.
Take anaemia testing, for example. A full blood count can show normal haemoglobin levels even in early iron deficiency, because your body is still compensating. By the time the test turns abnormal, you may have been iron-depleted for months, explaining the fatigue, breathlessness, and brain fog you've been experiencing.
Similarly, early autoimmune conditions, subtle hormone imbalances, and many nutritional deficiencies can exist beneath the radar of standard blood panels.
When "normal" results deserve a second look
There are several situations where normal blood tests warrant further investigation:
Your symptoms are persistent and affecting your daily life
If you're exhausted despite sleeping well, breathless without obvious cause, experiencing unexplained weight changes, or simply not functioning as you should, don't let a normal blood test close the door on further investigation. Symptoms are information, and persistent symptoms deserve answers.
You're at the extreme end of normal
A thyroid function test where your TSH is 4.8 (just inside the normal range of 0.5–5.0) might be perfectly fine for some people, but if you have classic hypothyroid symptoms and a family history of thyroid disease, that "high normal" result could be significant.
The tests don't match your clinical picture
Sometimes the wrong tests are ordered. Standard blood panels typically include basic checks like full blood count, kidney and liver function, and perhaps thyroid hormones. They won't pick up vitamin B12 deficiency unless specifically requested, won't detect most autoimmune conditions, and won't identify problems with cortisol, testosterone, or other hormones unless those specific tests are done.
There are red flag symptoms
Some symptoms should prompt urgent investigation regardless of initial blood results:
Unexplained weight loss
Persistent fever or night sweats
Lumps or swelling that won't go away
Changes in bowel or bladder habits lasting more than a few weeks
Chest pain or significant breathlessness
Neurological symptoms like weakness, numbness, or visual changes
These warrant prompt medical review and often require imaging, specialist tests, or referral, not just blood work.

What to do when you're told "everything's normal"
If your blood tests are normal but you know something isn't right, here are your next steps:
Ask for a detailed explanation
Don't settle for "it's all fine". Ask your doctor to go through the actual numbers with you. Where do you sit within the ranges? Have any results changed compared to previous tests? Are there specific markers that weren't tested?
Request a copy of your results
You have a legal right to access your medical records in the UK. Getting a copy of your blood results allows you to review them, track trends over time, and seek a second opinion if needed.
Consider whether additional tests might help
Depending on your symptoms, you might benefit from:
More detailed thyroid testing (including antibodies)
Vitamin levels (B12, folate, vitamin D)
Iron studies (not just haemoglobin)
Hormone panels
Inflammatory markers
Coeliac screening
Autoimmune antibodies
Seek specialist input
If your symptoms are complex, persistent, or your GP is unsure what's causing them, a consultant physician can provide a more detailed diagnostic assessment. We're trained to spot patterns that might not be obvious from standard tests, and to arrange more sophisticated investigations when needed.
Getting to the bottom of it
The gap between "normal test results" and "feeling normal" is where good medicine happens. It requires a doctor who listens carefully to your symptoms, understands the limitations of testing, and is willing to dig deeper when standard investigations don't provide answers.
Blood tests are powerful tools, but they're just one piece of the puzzle. Your experience of your own body, the fatigue that's changed your life, the breathlessness that's stopped you exercising, the brain fog that's affecting your work, is valid information that deserves proper investigation.
If you're stuck with normal blood tests but ongoing symptoms, don't give up. There's almost always an explanation, and with the right expertise and persistence, most patients do eventually get answers.
If you're struggling with unexplained symptoms or feel your blood test results don't match how you're feeling, you can book a private consultation with Dr Paraiso. As a consultant physician, I specialise in diagnostic uncertainty and complex symptoms, and can arrange appropriate investigations, interpret results in context, and develop a clear plan to get you back to feeling well. Consultations are available in Salford, Greater Manchester, or online.
This article provides general information only and is not a substitute for personal medical advice. If you are unwell or worried about a symptom, please speak to a healthcare professional. Call 999 or attend A&E immediately if you have severe chest pain, trouble breathing, signs of stroke, feel very unwell or think it is an emergency.

Comments